Structural Biochemistry/Cell Signaling Pathways/Endocrine System
The endocrine system consists of ductless glands that work together and secrete different hormones to regulate the human body. As an information signal system, hormones regulate many functions of an organism.
There are many types of signaling involved in the endocrine system including: autocrine, paracrine, and juxtacrine. Autocrine hormones act on the secreting cell itself, paracrine hormones act only on neighboring cells, and juxtacrine hormones act either on the emitting cell or adjacent cells.
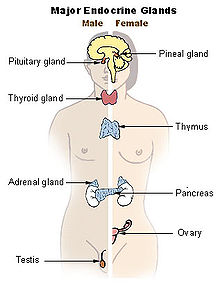
The number of glands that signal one another in a sequence is called an axis. The typical endocrine glands are the pituitary, thyroid, adrenal glands, pancreas glands, ovaries, and testes.
Pituitary Gland
editAlso known as the hypophysis, the pituitary gland is about the size of a pea weighing 0.5g and is located at the bottom of the hypothalamus at the base of the brain and rests in a small, bony cavity (sella turcica) covered by a dural fold (diraphragma sellae). It is considered the master gland as it secretes hormones regulating homeostasis. It is functionally connected to the hypothalamus by the median eminence.
Anterior pituitary (adenohypophysis) synthesizes and secretes important hormones such as: ACTH, TSH, PRL, GH, endorphins, FSH, and LH and are released under the influence of the hypothalamus through the hypothalamic-hypophyseal portal system. Hypothalamic hormones travel along axons until they’re released from terminal arborizations into the blood vessels of the hypothalamic-hypophyseal portal system. They are then carried into the adenohypophysis where cells are stimulated with hormone-specific receptors which trigger a release of a certain hormone. The anterior pituitary gland is divided into regions known as the pars tuberalis, pars intermedia, and pars distalis.
Posterior pituitary (Neurohypophysis) stores and releases oxytocin and antidiuretic hormone (ADH and AVP). Oxytocin has a positive feedback loop and is released from the paraventricular nucleus in the hypothalamus. ADH (vasopressin) and AVP (arginine vasopressin) is released from the supraoptic nucleus in the hypothalamus. ADH is controlled by the blood osmolarity. As blood osmolarity increases, the signal leads to increased ADH release from supraoptic nucleus. If a concentrated solution is perfused near the supraoptic and paraventricular nuclei, that can also signal an increase in ADH release.
The process by which hormones are released in the neurohypophysis and the andenohypophysis are quite similar. In the neurohypophysis, the hormones are synthesized in the supraoptic and paraventricular nuclei of the hypothalamus (in the brain- most of it is synthesized in the supraoptic nucleus). These hormones are then transported to the posterior pituitary where it is stored in and released from the terminals of these neurons whose cell bodies are in the hypothalamic nuclei. These terminals are like the synaptic terminals between neurons, except for the fact that they release their "transmitter" into the bloodstream rather than onto other neurons. Finally, release of these hormones occur when electrical activity increases in the hypothalamic cells that project into the neurohypophysis. In the adenohypophysis, the release of hormones synthesized and stored by the cells is controlled by local hormones produced by cells in the hypothalamus. These hypothalamic hormones (called release hormones or release-inhibit hormones) are all peptides. These releasing hormones are transported along axons of the hypothalamic neurons, where they are released from terminal arborizations that resemble synapses. The synapses end on the blood vessels of a portal system in the median eminence of the hypophyseal stalk (a portal system being a collection of veins that connect capillary beds in two organs rather than connecting the capillary bed in an organ with the rest of the circulation). The releasing hormones are then carried by the blood to the adenohypophysis where they stimulate cells with hormone-specific receptors to release their stored hormones. Intermediate lobe produces melanocyte-stimulating hormone (MSH).
Functions: The pituitary hormones help control: growth, blood pressure, breast milk production, sex organ functions in both sexes, thyroid gland function, metabolism, water regulation, secretion of ADH to control water absorption in the kidneys and temperature regulation.
Thyroid Gland
editLocated in the neck below the thyroid cartilage, the thyroid controls the rate at which the body burns energy, makes proteins, and controls sensitivity to hormones. The thyroid produces its own hormones including thyroxine (T4) and triiodothyronine (T3) which regulate the rate of metabolism and affect the growth and functional rate of other systems in the body.
Controlled by the hypothalamus and pituitary gland, the thyroid gland gets its name from the Greek "shield" after the shape of the thyroid cartilage.
The most common problems involving the thyroid gland include: hyperthyroidism and hypothyroidism. Hyperthyroidism is an overactive thyroid while hypothyroidism is an underactive thyroid.
Parathyroid Gland
editThe important hormone is parathyroid hormone (PTH) and is regulated by calcium in blood. Its main function is to raise blood calcium level. It is secreted by parathyroid glands, causes bone to release Ca2+ in the kidneys. PTH also stimulates the kidneys to activate vitamin D, promoting intestinal uptake of Ca2+ from food.
Adrenal Gland
editAlso known as the suprarenal gland, the star-shaped adrenal gland sits on top of the kidneys and is responsible for releasing hormones in conjunction with stress through the synthesis of corticosteroids and catecholamines using cortisol and adrenaline, respectively.
The adrenal cortex is vital to the synthesis of corticosteroid hormones from cholesterol. The source of cortisol and corticosterone synthesis is the hypothalamic-pituitary-adrenal axis. Under normal unstressed conditions, the human adrenal glands produce the equivalent of 35–40 mg of cortisone acetate each day. They also have other functions which include producing androgens (like testosterone)and regulating water and electrolyte concentrations via secretion of aldosterone. The adrenal cortex is regulated by neuroendocrine hormones secreted by the pituitary gland renin-angiotensin system, and hypothalamus.
The three layers of the adrenal cortex are: zona glomerulosa, zona fasciculata, and zona reticularis. Zona glomerulosa is the site for production of mineralocorticoids which affect the body's sodium homeostasis. Zona fasciculata produces glucocorticoids in humans. Cortisol secretion is simulated by adrenocorticotropic hormone (ACTH) from the anterior pituitary. In the absence of ACTH, zona fasciculata secretes a basal level of cortisol. Zona reticularis produces mainly dehydroepiandrosterone (DHEA) and DHEA sulfate.
The adrenal medulla is the core of the adrenal gland and is surrounded by the adrenal cortex as it releases secretions directly into the blood stream. The chromaffin cells of the medula are the main source of circulating water-soluble catecholamines derived from the amino acid tyrosine: adrenaline (epinephrine) and noradrenaline(norepinephrine). This is party of the fight-or-flight response initiated by the nervous system.
Arteries and veins supply blood to the adrenal gland. The superior suprarenal artery is provided by the inferior phrenic. The middle suprarenal artery is provided by the abdominal aorta and the inferior suprarenal artery is provided by the renal artery. The right suprarenal vein drains the inferior vena cava and the left suprarenal vein drains the left renal vein also known as the left inferior phrenic vein. The suprarenal veins may form anastomoses ( the branching out and reconnection of blood vessels) with the inferior phrenic veins.
Pancreas Gland
editSituated deep within the abdomen between the stomach and the spine, it is known as both the double gland and the mixed gland because it has both endocrine and exocrine functions. As an endocrine gland, it secretes hormones into the bloodstream. When it comes to its function as an exocrine gland, it plays a pivotal role in the secretion of enzymes to help break down carbohydrates, fats, proteins, and acids in the duodenum. More importantly, the pancreas gland secretes the insulin hormone, which regulates sugar metabolism. Too little insulin would result in high blood sugar levels in addition to muscle and body weakness (a condition known as diabetes).
Observing the functionality of the pancreas gland reveals its involvement in the production of chemicals that are critical to proper digestion and blood sugar regulation. Besides its role in the secretion of the body's important enzymes, the pancreas gland also creates digestive juices as a member of the exocrine system. These fluids play a key role in breaking down the nutrients that the stomach acids were incapable of metabolizing. The juices initially are alkaline in the pancreas but as they make their way through the stomach where they meet other substances, they become acidic.
Ovaries
editThe ovaries, situated in the pelvis with each ovary on opposite sides of the uterus, are a pair of female reproductive organs. To give you a sense of the shape and size of an ovary, we can consider it quite similar to the size and shape of an almond. Ovaries specifically have two functions: they produce eggs and just like the other glands of the endocrine system, they produce female hormones.
The ovaries are in fact the main source of female hormones, which include estrogen and progesterone. These hormones play a pivotal role in controlling the development of female body characteristics, such as the breasts, body shape, and body hair. More importantly, the ovaries also regulate the menstrual cycle and pregnancy.
Testes
editThe testes is the male reproductive organ held responsible for the production and storage of millions of tiny sperm cells. The testicles are oval-shaped and can grow to about five centimeters in length and 3 centimeters in diameter. The testes do indeed play a pivotal role in the endocrine system due its production of hormones, namely testosterone. As a young man reaches puberty, his testes actually produce more and more of this hormone. More importantly, this hormone causes boys to have deeper voices, bigger muscles, grow facial and body hair, and stimulate the production of sperm.
Hypothalamus
editIt is a portion of the brain containing some small nuclei with a variety of functions. It plays a central role in integrating the endocrine and nervous systems. The hypothalamus is located below thalamus, just above the brain stem. The hypothalamus receives information from nerves throughout the body and from other parts of the brain. Signals from the hypothalamus travel to the pituitary gland, which is located at the base. Some produce directacting hormones that are stored and released from the posterior pituitary. Other hypothalamic cells produce hormones that are transported by portal blood vessels to the anterior pituitary. These hormones either promote or inhibit the release of hormones from the anterior pituitary.
The way in which the hypothalamus promotes or inhibits the release of hormones from the anterior pituitary is through the use of a portal vein system and hormone-releasing hormones. Hormone-releasing hormones include, Growth hormones, Prolactin, Folicle-stimulating hormone, Luteinizing hormone, Thyroid-Stimulating Hormone, and ACTH. These hormones are released by the anterior pituitary upon promotion of their release via hormone-releasing hormones such as antidieuretic hormone, ADH. Once these hormones reach the anterior pituitary gland via the portal vein connected the hypothalamus and the gland, the hormones are secreted into the bloodstream and taken up by their specific receptors throughout the body.
The effect of any hormone on a cell depends on the cell's intracellular machinery. Hormones only affect the specific receptors to their appropriate receptor molecules in their membranes. Their is little effect of these hormones on other types of cells due to receptor specificity. An example of this is that in the smooth muscle fibers of the blood vessel walls, catecholamines produce contraction but in the liver, catecholamines make it possible for the breakdown of glycogen and the release of glucose into the bloodstream.
Hormones
editTropic hormones It is a hormone that regulates the function of endocrine cells or glands. It is also produced and secreted by anterior pituitary that target endocrine glands. Tropic hormones include TSH, follicle-stimulating hormone (FSH), luterinizing hormone (LH), and adrenocorticotropic hormone (ACTH). The main target ofFSH and LH are testes or ovaries.
Nontropic hormones include prolactin (PRL) and melanocyte-stimulating hormone (MSH).
Growth hormone is secreted by the anterior pituitary and stimulates growth through tropic and nontropic effects. The major targets are liver, bones, and other tissues.
Some hormones have very specific targets while others affect essentially all cells of the body. Most hormones belong to one of a few basic families: the peptides, the amino acid derivatives, and the proteins. Many endocrine glands secrete more than one hormone each. When this is the case, the hormones secreted by a gland belong to the same family. In general, each family operates by a characteristic mechanism to regulate the function of target cells. All of them must first bind to receptor molecules that specifically recognize hormones. Protein and peptide hormones bind to membrane surface receptors and through a series of reactions involving small cytoplasm molecules called "second messengers" and enzymes called protein kinases. These hormones modify the activity levels of proteins within the cytoplasm by causing them to be phosphorylated on particular amino acid residues. Also, these peptides and protein hormones are charged at normal pH and cannot cross cell membranes. These hormones therefore must bind to the extracellular domain of g-protein coupled receptors. On the other hand, steroid hormones and thyroid hormones are hydrophobic. Due to their physical properties, steroid hormones and thyroid hormones must bind to intracellular receptors, which allow them to move into the nucleus bound to their receptors, directly affecting the transcription of genes.
When level of hormone is too high, the normal effects of hormones are exaggerated. This effect is known as hypersecretion. The causes of hypersecretion include benign and malignant tumors of the endocrine glands. Imbalance of hormones in the body can also come from outside of the body, known as exogenous hormones or agonists. The introduction of exogenous hormones in the body is known as iatrogenic. For example, when certain hormones such as cortisol in the body is introduced, it causes the shutdown of the secretion of hypothalamus and anterior pituitary glands. This causes the loss of cell mass, called atrophy. In contrast, hormone deficiency in the body is called hyposecretion. The main cause of hyposecretion is from atrophy of the gland due to a certain disease process.
The specificity of the response to any hormone lies in the properties of the receiving cells and not in the delivery of those hormones to the cells. Only the cells with the appropriate receptor molecules respond, even to the steroid hormones that will dissolve through the membranes of all cells. The effect that any hormone has on any particular cell depends upon the cell's own intracellular machinery. When a hormone binds to its specific receptors on different kinds of cells, the effect depends upon the nature of the cell.
Hormonal control
editHormonal control involves a negative feedback loop and thus homeostasis within the body. Many types of hormones exist in the body and thus many different feedback loops exist for the systems. Some of them are very simple, others are very complex.
A simple example of hormonal control is the feedback loop for Insulin. Insulin is released into the bloodstream via blood cells of the pancreas, and it controls the rate at which most cells remove glucose from the bloodstream. Insulin is synthesized and stored in pancreatic beta cells. The synthesis and the release of insulin are triggered by the increase of glucose in the bloodstream. Other signals such as an increase in amino acid concentration in the blood, the presence of several other hormones, and neural control, have an effect on the increase of insulin into the bloodstream. Hormone signals are always terminated by either the binding of the hormone to its specific receptor and the breakdown of the hormone via bloodstream enzymes.
References
editD. Silverthorn. (2010). Human Physiology 6th Edition. San Francisco, California: Pearson